THANK YOU FOR VISITING SWEATSCIENCE.COM!
My new Sweat Science columns are being published at www.outsideonline.com/sweatscience. Also check out my new book, THE EXPLORER'S GENE: Why We Seek Big Challenges, New Flavors, and the Blank Spots on the Map, published in March 2025.
- Alex Hutchinson (@sweatscience)
***
The latest study from Paul Williams’s National Runners’ Health Study appears in the new issue of the American Journal of Cardiology. I like Amby Burfoot’s pithy summary of the results: “The faster you are, the longer you’ll live.”
On the surface, the study is very simple. Williams looked at the 10K PBs of 29,721 men in his survey-based study, and then followed up 7.7 years later to see who had suffered heart attacks, angina, or died of factors related to heart disease. Not surprisingly, the faster subjects were less likely to suffer any of the negative outcomes:
Each meter/second increment in running performance was associated with a 44% lower risk for CHD death and nonfatal myocardial infarction, a 54% lower risk for nonfatal myocardial infarction, a 53% lower risk for angina pectoris, and 32% lower risk for revascularization procedures (percutaneous transluminal coronary angioplasty or coronary artery bypass grafting).
(An increase of one meter/second represents the difference between, for example, a 44-minute 10K and a 35-minute 10K.)
Pretty obvious, right? But there’s a twist: the results stay roughly the same even when you control for physical activity. In other words, if you’re trying to predict how likely you are to have a heart attack, it doesn’t matter how much you run, just how fast you are. In a sense, this is sort of bad news. We’ve generally assumed that being fit and being active are essentially the same thing. But Williams notes that “up to 70% of the variation in aerobic capacity is inherited in humans,” so some people need to be far more active than others to reach the same level of fitness (or running speed). This ties into an ongoing debate about “fatness versus fitness”: researchers like Stephen Blair argue that being active is more important than being skinny. But the new data goes further and argues that being active isn’t enough — you actually have to be aerobically fit, as measured by something like a 10K race or a VO2max test.
This doesn’t mean we’re captive to our genetic fates; it just means we may need to rethink how we approach exercise, according to Williams:
The present findings are relevant to the formulation of public health guidelines. Current guidelines primarily target the volume of physical activity rather than cardiorespiratory fitness, whereas fitness-targeted guidelines would place greater emphasis on vigorous exercise and interval training.
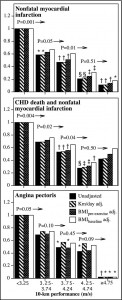
So this sounds like another argument for “high-intensity interval training,” which is already getting lots of press. But Williams makes a further distinction. These days, most experts are touting the time-saving benefits of interval training — i.e. get all the benefits of a 45-minute run by doing four 30-second spurts on an exercise bike. Instead of using intervals (and other forms of vigorous training) to reach the same fitness level in less time, he argues, we should spend the same amount of time and reach higher fitness levels. Want motivation? Here are the graphs of relative risk,for speeds ranging from slower than 51 minutes for 10K on the left to faster than 35 minutes on the right:

One Reply to “10K time predicts risk of heart disease, independent of training”
Comments are closed.